Our Eye Clinic
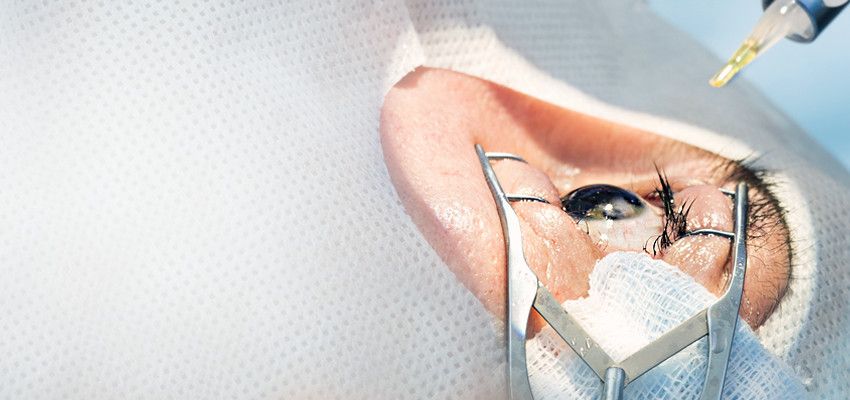
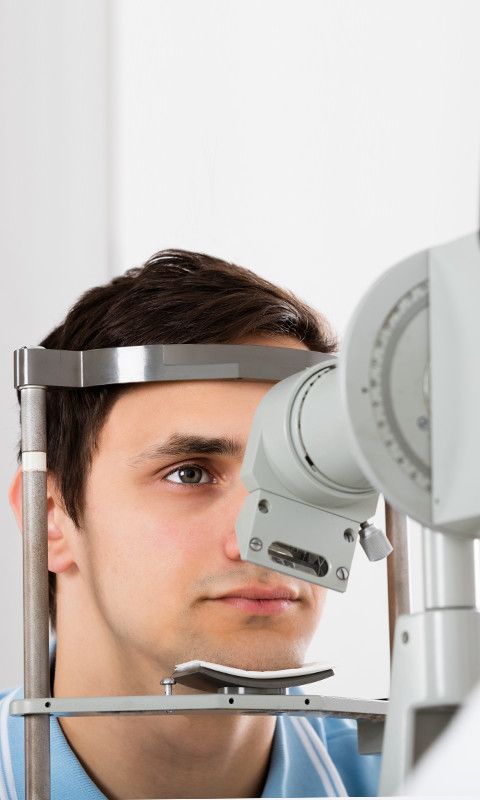
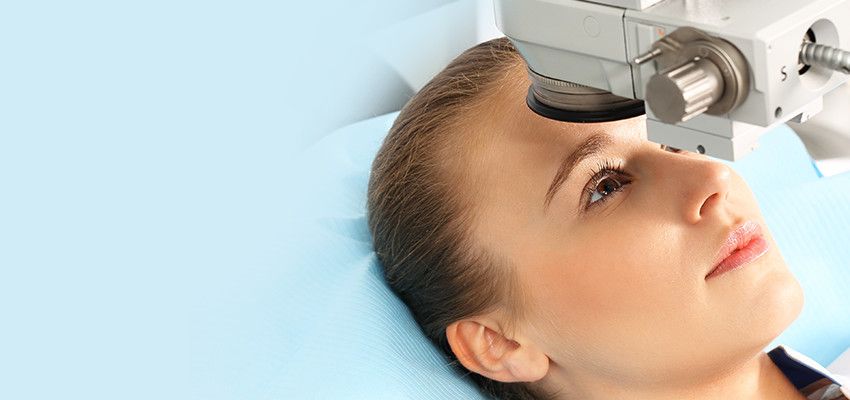
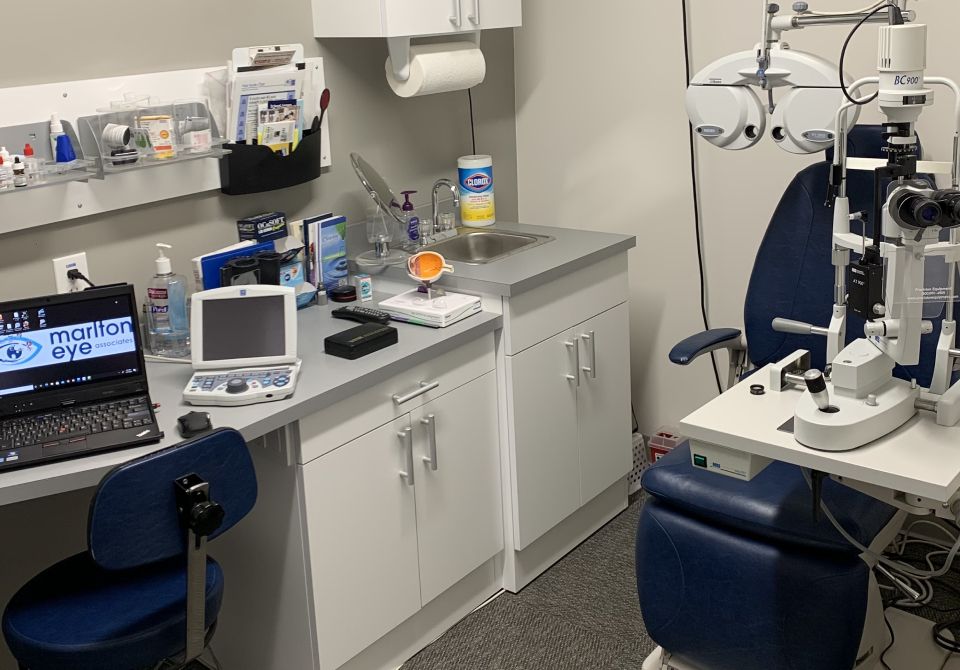
We specialize in caring for all your vision needs. We handle everything from eye exams and hard-to-fit contact lenses to computer vision problems, specialty lenses, and co-management of eye surgery. We're a sincere company with a straightforward vision. With us, vision care goes far beyond a simple eye examination.